Health
Tips for managing insomnia in children with autism spectrum disorder (ASD)

Highlights
- Up to 80% of children with ASD have sleep difficulties
- This could last into adulthood if left untreated, says Cleveland Clinic Children’s researcher.
- Certain behavioural-based approaches suggested alongside short-term use of medications, including melatonin and iron supplements, recommended.
Dubai: Behavioural therapy and certain short-term medication could help alleviate insomnia in children with autism spectrum disorder (ASD), according to an expert.
Cynthia Johnson, PhD, Director of Cleveland Clinic Children’s Center for Autism and Professor of Paediatrics, said insomina affects 8 out of 10 children ASD. She explained that behavioural-based approaches and short-term use of medications, such as melatonin supplements, may be helpful.
Behavioural approaches
Behavioural-based approaches, she said, involve the following:
· Environmental modification,
· Establishment of stimulus control,
· Skill building, and
· Leveraging principles of reinforcement.
The good news, said Dr. Johnson, is that several research projects where she has been involved in show behavioural strategies can make a significant difference in reducing insomnia.
“Short-term use of medications such as melatonin supplements might also be considered,” she added.
Sleep problems in individuals with ASD have been associated with poor social interaction, problems in communication, and overall autistic behaviour.
Family involvement
Many of the strategies can be successfully delivered by the child’s family, said Dr Johnson, who made the remarks on the occasion of World Autism Day (April 2).
The specialist says insomnia in kids with ASD can have a negative impact on both the wellbeing of sufferers and the wellbeing of their families.
What is autism spectrum disorder (ASD)?
ASD is a chronic nervous system condition brought on by genetic, metabolic, or other biological causes. The World Health Organisation (WHO) estimates that one in 160 kids worldwide has ASD. As a developmental disability, autism can cause significant emotional, social and behavioural dysfunction. Sleep disorders co-occur in a huge portion of the patients with ASD.
Insomnia: Common in children with ASD
“Insomnia is significantly more common in children with ASD compared with the general paediatric population, and also persists for a longer period, carrying through to adolescence and adulthood, if left untreated,” says Dr Johnson.
She lists a number of behavioural traits of children with ASD, which may raise the risk of sleeplessness, including:
· Rigidity and insistence on sameness,
· Inadequate communication,
· Anxiety, and
· Hyperactivity.
Biological risk factors
Biological risk factors can also lead to certain effects — such as variations in brain development, changed melatonin secretion, or mutations in genes that control circadian rhythms.
In addition, clinical variables including untreated gastrointestinal issues and negative pharmaceutical side effects might also worsen sleep disorders.
Commenting on the impact of insomnia on a child, Dr. Johnson says, “Sleep plays an important role in the growth, development and wellbeing of children.”
Studies have shown a lack of adequate, quality sleep can have negative effects on attention, daytime behaviour and the regulation of emotions, and could even impact children’s cardiovascular, metabolic and immune systems.
In addition to the child, the family will be impacted, Dr. Johnson adds.
“The child’s insomnia can affect other family members’ ability to function because, if the child is not sleeping, everyone’s sleep can be disturbed. This adds to parental stress in the long term, with parents dedicating a great deal of time to strategizing on how to get the child to sleep.”
Varying presentation
Insomnia presents in children with ASD varies from child to child, she said, adding: “Sleep problems may be irregular, cyclical or constant and they can take many forms.
For example, the child might resist bedtimes, or insist on elaborate bedtime routines, or might have difficulty falling asleep or staying asleep, or the child might wake up too early.”
Low ferritin levels is also a factor seen behind insomnia in children with ASD.
What can be done?
Interventions are not “one size fits all” solutions, she said.
“As each child responds differently to treatment strategies, parents should work together with an expert in ASD sleep disorders and behavioural interventions.
“The aim is to approach the problem collaboratively and systematically, exploring the day and nighttime routines of the child and family, and testing various preventative and skill-building strategies until the best solution is found.”
Dr. Johnson points out that treatment approaches are continuing to evolve, and new therapies have been found over the past decade and a half.
Behavioural-based approaches, supplements
Behavioural-based approaches involve environmental modification, establishment of stimulus control, skill building and leveraging principles of reinforcement.
Short-term use of medications such as melatonin supplements might also be considered, she says.
Studies also show that low ferritin levels can also be a factor in sleep disorders.
In 2013, a retrospective chart review of data involving 9,791 children with ASD conducted by researchers led by Julie Youssef, of the Department of Neurology, Boston Children’s Hospital, Harvard Medical School, found that significantly low serum ferritin levels were associated with several sleep disorders — including:
· Periodic limb movements during sleep,
· Sleep fragmentations, and
· Poor sleep efficiency.
Ferritin is a storage form of iron. The sudy found that iron supplementation was be effective in the treatment of low ferritin with sleep disorders.
Also, in a 2012 study led by Lynn M. Trotti, of the Department of Neurology, Emory University School of Medicine in Atlanta recommends iron therapy for low ferritin level below 50 ng/mL for children with ASD facing sleep disorders.
Further research
A study, published in 2007 in Paediatric Neurology, conducted an open-label trial of oral iron supplement (6 mg elemental iron/kg/day) for 8 weeks in children with autism and showed improvement in sleep, with an increase in serum ferritin level.
However, potential side effects were cited, including “metallic” taste, vomiting, nausea, constipation, diarrhoea, and black/green stools.
Antipsychotics, antidepressants, and alpha (α) agonists have also generally been used alongside melatonin.
Experts, however, said that given the limited evidence for psycho-pharmacological treatments in autism, behavioural interventions are considered a primary mode of treatment.
Still, further research and information are needed to guide and individualise treatment for this population group.
Gulf News
Health
Obesity drug shows promise in reducing belly and liver fat
Boehringer Ingelheim said on Sunday its experimental obesity drug cut visceral and liver fat while minimizing loss of lean mass in a late-stage study, data showed, bolstering its case for benefits beyond weight loss as competition in obesity drugs intensifies.
The drug, survodutide, was licensed from Denmark’s Zealand Pharma (ZELA.CO), opens new tab. An injectable that mimics the proteins GLP-1 and glucagon to create a feeling of fullness, its weight-loss trial results were announced in April, showing patients lost an average of 16.6% over 76 weeks.
Analysis of a group of patients who had MRI measurements at the start and end of a 76-week trial showed that survodutide reduced harmful abdominal fat by up to 34% and liver fat by up to 63.1% from the baseline, Boehringer said.
Analysts have said the weight-loss numbers were broadly comparable to existing GLP-1 injections from Novo Nordisk (NOVOb.CO), opens new tab and Eli Lilly (LLY.N), opens new tab and below newer rivals in development, and that the company needed to differentiate the drug’s benefits.
Lean mass accounted for no more than 10.8% of the change in body composition at the highest dose of 6 milligrams, suggesting the weight loss was driven mainly by fat reduction.
The drug’s effect on liver-fat reduction and preservation of lean mass are central to whether it will be able to stand out commercially, alongside tolerability and how long patients stay on the drug. Detailed data from the study could help Boehringer make a stronger case that survodutide should be judged not only by pounds lost but by where weight is lost.
“We believe survodutide will become an important new option at the intersection of obesity and liver disease, two conditions that are deeply connected but rarely addressed together,” said Boehringer executive Shashank Deshpande, who leads the company’s human medicines business.
Boehringer acquired the rights in 2011 to solely develop and commercialise survodutide from Zealand, which is entitled to royalty payments on global revenue.
PATIENTS WITH LIVER DISEASE BENEFIT
In a separate late-stage study of overweight or obese patients with a fatty liver disease called MASLD, survodutide met both its main goals.
After 48 weeks, up to 84.2% of patients on the drug showed a liver fat reduction of at least 30%, compared with 24.3% for those on placebo. Patients on survodutide also lost up to 12.2% of their body weight, versus 1% for placebo.
In 61% of the patients the drug helped achieve liver fat normalization, or a liver fat content below 5%, compared with 5.7% on placebo.
U.S. biotech Altimmune (ALT.O), opens new tab is also developing a drug that targets both the appetite-suppressing gut hormone, GLP-1, and glucagon.
Survodutide is also being tested in other late-stage studies, including for patients with fatty liver disease and fibrosis.
REUTERS
Health
Millions with breast cancer could safely skip chemotherapy
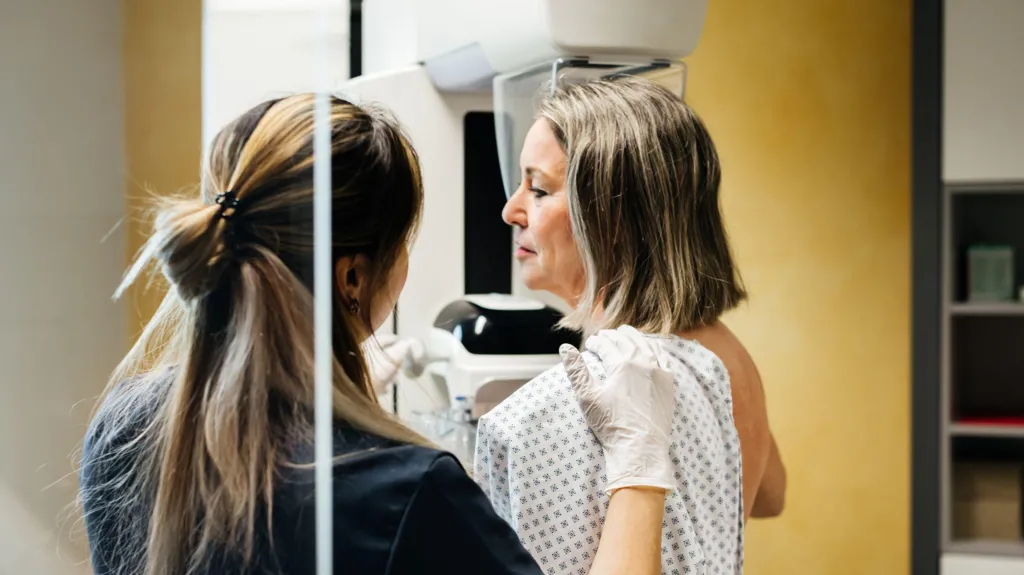
Millions of people with breast cancer could safely avoid chemotherapy as scientists have developed a DNA test that can distinguish between patients who are likely to benefit from the treatment and those who are not, according to trial results.
The international study found that more than two-thirds of its participants could be spared the side of effects of chemotherapy and treated with hormone therapy alone.
Chemotherapy can cause fatigue, nausea, hair loss, a weakened immune system and fertility issues.
The study, led by University College London (UCL), involved more than 4,000 newly diagnosed patients over the age of 40 in the UK, Norway, Sweden, Australia, New Zealand and Thailand.
Scientists used a gene test called Prosigna to measure the activity of 50 genes involved in breast cancer growth and calculate a patient’s risk of the disease returning.
Those who received a low score – two-thirds of the group – were not treated through chemotherapy. The five-year survival rate of their group was 93.7%, compared with a 94.9% rate among patients who received chemotherapy as part of their care.
The primary treatment for breast cancer is usually surgery to remove tumours. Chemotherapy is often recommended afterwards to diminish the risk of return.
It is also regularly offered to people with early-stage breast cancer that has spread to the nearby lymph nodes.
Clinicians are concerned the treatment provides little benefit to those with the most common type of breast cancer, UCL said.
The university said more than 5,000 NHS patients a year could avoid chemotherapy as a result of the trial.
Karen Bonham, from Cardiff, took part in the trial and said the results are an “immense relief” and feel “like Christmas”.
The 64-year-old avoided chemotherapy thanks to the Prosigna test and has instead received radiotherapy and hormone therapy over eight years.
“Cancer diagnosis and treatment can be shocking,” she said.
“It certainly propels you into a world of uncertainty. Life priorities realign – you simply want to survive.”
The findings of the study will be presented at the world’s largest cancer conference, the American Society of Clinical Oncology’s annual meeting, in Chicago, United States, on Saturday.
Professor David Miles, a leading cancer specialist, described the findings as “practice-changing”.
“We can now confidently predict many patients will get no benefit at all, and therefore there’s no need for them to have the chemotherapy,” he told BBC’s Newshour.
He added that the test would allow doctors to “confidently define a large population of women who simply aren’t going to benefit and don’t need to go through all that unpleasantness for no benefit at all.”
“We used to give chemotherapy to 100 women to benefit 10, knowing that 90 didn’t need it,” he said.
Tanya Hutson, who was diagnosed with breast cancer in 2022 and had chemotherapy as part of her treatment, called the new DNA test “absolutely amazing”.
“It just proves what happens when money is put into research,” she said, adding that chemotherapy had been “brutal”.
“For all these people out there who don’t need it but are still getting it – it’s an absolute game changer.”
It is not known whether the findings apply to people under the age of 40, with a result still several years away, according to UCL.
BBC
Health
How to stay healthier in your 70s by starting in your 30s
By the time you reach your eighth decade of life, the chances are that you’ll probably be feeling weaker, stiffer, and perhaps a little less cognitively sharp than in your younger years. Your sleep patterns might have changed so that you feel drowsier in the evenings and then wake earlier. Most concerningly, going by population averages, it’s likely that you will be dealing with at least one chronic health condition.
Yet researchers, now more than ever, are convinced that this is not an inevitability. “Based on what we now know, most people could expect to live to 90 or even 95 in good health if they were to optimise their lifestyle,” says Eric Verdin, president and chief executive of the Buck Institute for Research on Ageing in California. “And that’s very far from where we are, where most people live to 65 or 70 in good health, and then become ill and suffer all the indignities of old age.”
While Verdin says that it’s never too late to improve your health at any age through making positive lifestyle adjustments, whether that’s exercising more, eating better or cutting back on alcohol, you will likely fare best if you start sooner. In particular, researchers have highlighted your 30s as a key decade when a number of physiological systems, whether that’s muscle mass and strength, bone density or metabolic regulation, begin to show the first subtle age-related changes.
“It does highlight this period as an important opportunity to reinforce behaviours that build long-term resilience,” says João Passos, a professor of physiology at the Mayo Clinic’s Kogod Center on Ageing, based in Minnesota.
To understand what might be possible, researchers studying the ageing process like to focus on groups of people who buck the ordinary trends. One example is masters athletes, individuals aged over 35 who still compete regularly in sporting competitions, whether that’s running, cycling or other sports, often continuing into their 60s and beyond.
Paul Morgan, a senior lecturer in nutrition and metabolism at Manchester Metropolitan University, notes that many of these athletes display a very different ageing trajectory to the rest of us, characterised by a higher peak in cardiovascular function and muscle strength and function, followed by a delayed decline. As a result, he says that many of them manage to avoid loss of mobility and independence for much longer in later life. “They have this additional reserve which acts as a protective barrier through the middle stages of life,” says Morgan.
We can all learn from this. To give us the best chance of ageing well, Morgan says that we should aim to hit the highest peak that we can in our 30s, particularly when it comes to aerobic capacity (the maximum amount of oxygen your body can use during exercise), flexibility, and muscle strength.
One of the biggest risks for anyone over the age of 70 is tripping and falling, which is linked to a loss of agility and a decreased range of motion in the joints. “I always see the muscle groups in the lower limbs that are responsible for locomotion as having the biggest role to play in maintaining independence, and with that, good health in later life,” says Morgan. “So that’s especially important to focus on.”
Playing sport is an excellent way to achieve this. Research has shown that taking part in racquet sports such as tennis or badminton has a consistent association with extended lifespan, while a 2025 Japanese study highlighted the benefits of cycling, with older adults who cycle regularly being less likely to need long-term care or die prematurely.
Running for more than 75 minutes per week has also been found to slow certain aspects of the ageing process, but you might want to think again when it comes to running marathons. There is some evidence that pushing your body to extremes can actually accelerate some aspects of biological ageing, although this remains less well understood.
On the other hand, one study found that as little as five minutes of moderate to vigorous physical activity per day can help slow brain ageing, and according to Aditi Gurkar, an assistant professor of medicine at the University of Pittsburgh in the US, we can all get some of the healthy ageing benefits through following relatively simple steps. “Even a brisk 15-minute walk after a meal can make a meaningful difference,” she says.
Building your brain’s reserve
Just as we can protect and strengthen our muscles and cardiovascular system in our 30s, we can also do the same for our brain. Maintaining good dental health through regular checkups, a good brushing routine, not smoking, and limiting intake of sugary foods can make a surprising difference.
This is based on numerous studies which have repeatedly linked the development of periodontal disease, a gum condition characterised by elevated inflammation, with a heightened risk of cognitive decline in later life. This is thought to be due to the chronic impacts of systemic inflammation on the brain.
Your 30s could also be the decade to begin reducing your alcohol consumption. Drinking alcohol is linked to changes in gene expression in the body which accelerate ageing. Alcohol is also a key disruptor of sleep, and Verdin highlights consistent sleeping patterns as being key for avoiding age-related brain shrinkage and lowering dementia risk in decades to come. This includes making sure you go to sleep and wake up at the same time every day, known as sleep regularity. Not only does sleep allow the body to focus on repairing cells, it also gives people the energy and motivation to pursue a healthy lifestyle.
“Even if you’re lacking sleep for one night, your metabolism changes, and your willpower to do all the things that are keeping you healthy goes away,” he says.
Because of the importance of maintaining a regular sleeping pattern, Verdin says he now uses an alarm clock each night – not to wake himself up, but to remind him to go to bed. “The reason for this is we’re circadian beings,” he says. “Our whole biology, from gene expression to metabolism is in synchrony with the 24-hour cycle, and so I tell people, going to bed at the same time each day helps your body to stay really well synchronised to all of this.” A good night’s sleep may not always be possible, however, as anyone raising young children in their 30s will know.
Finally, your 30s is probably a good time to begin taking nutrition a little more seriously. Verdin says that one of the best things we can do is to give our bodies more time during the day when we’re not actually eating, for example through intermittent fasting.
While many proponents of intermittent fasting recommend a so-called 16:8 split, where you fast for 16 hours of the day and compress your eating into an eight-hour window, Verdin says that we can achieve plenty of benefits through a more manageable 12:12 split. “Essentially when you’re fasting, that allows your body to focus not on digesting but on repairing,” he says. “I tell people, when you are eating, you are building. When you’re fasting, you are repairing.”
Consuming more fruit and vegetables at the expense of ultra-processed foods could also make a difference. Gurkar points to work that she and others have carried out showing that people who ingest higher amounts of dietary carotenoids – plant chemicals found in vegetables such as sweet potatoes and carrots, and fruits like mango and apricots – age more slowly, possibly because these chemicals can play a role in protecting our cells from a form of damage called oxidative stress.
Overall, Passos is convinced that the choices we make in early adulthood can have a lasting impact on how we age. He points to large studies which have tracked tens of thousands of people in the US for decades, such as the Framingham Heart Study and the Nurses’ Health Study, which reveal that people who maintain healthier lifestyles in midlife have lower risks of cardiovascular disease, cognitive decline and frailty – even decades later.
“By maintaining healthier behaviours in our 30s, we may prevent or delay subtle molecular and cellular changes that, if left unchecked, accumulate over time and contribute to functional decline in our 70s,” says Passos. “While I don’t believe that by doing this we can stop ageing, we can certainly shape its trajectory.”
While you may still feel somewhat invincible in your 30s, the steady tick of the ageing clock ultimately impacts us all. But if you cut out excessive alcohol, find a sport which you can keep playing into your latter years, set a regular sleeping pattern and give your body more breaks from constant eating, your heart, muscles, joints, and brain will all thank you in years to come.
BBC
-

 Discover5 months ago
Discover5 months agoIs February 2026 really a once-in -283-years MiracleIn?
-

 Entertainment4 months ago
Entertainment4 months agoNetflix to Livestream BTS Comeback Concert
-

 Football6 months ago
Football6 months agoAlgeria, Burkina Faso, Côte d’Ivoire win AFCON 2025 openers
-

 Health5 months ago
Health5 months agoNMC Royal Hospital, Khalifa City, performs rare wrist salvage, restoring function for young patient
-

 Health6 months ago
Health6 months agoBascom Palmer Eye Institute Abu Dhabi and Emirates Society of Ophthalmology Sign Strategic Partnership Agreement
-

 Health7 months ago
Health7 months agoEmirates Society of Colorectal Surgery Concludes the 3rd International Congress Under the Leadership of Dr. Sara Al Bastaki
-

 Lifestyle7 months ago
Lifestyle7 months agoSaudi Arabia Lifestyle Trends 2025: What You Need to Know About Fitness, Wellness, Healthy Eating & Self-Care Growth
-

 Health7 months ago
Health7 months agoBorn Too Soon: Understanding Premature Birth and the Power of Modern NICU Care


